Connect With Us
Blog

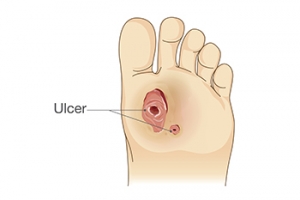
Causes and Care of Diabetic Foot Ulcers
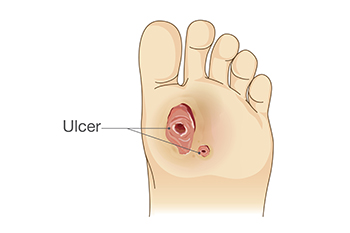
Diabetic foot ulcers are common complications that arise from prolonged high blood sugar levels, leading to nerve damage and poor circulation. These factors increase the risk of injury, as decreased sensation can prevent individuals from noticing cuts or blisters that may develop into ulcers. Caring for diabetic foot ulcers involves keeping the wound clean and covered, monitoring for signs of infection, and maintaining proper blood sugar levels to promote healing. Regular foot inspections and gentle cleaning with mild soap and water are essential. Risk factors for developing these ulcers include neuropathy, poor circulation, wearing improper footwear, and foot deformities. Maintaining a healthy weight and managing diabetes through diet and exercise can further reduce the risk. If you have diabetes and have developed a foot ulcer, it is suggested that you schedule regular appointments with a podiatrist who can effectively treat this condition.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Daniel Bell, DPM from Florida. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Pembroke Pines and Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
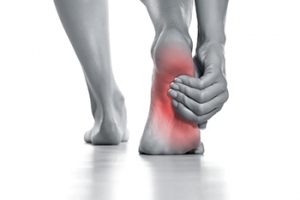
Facts About Heel Stress Fractures
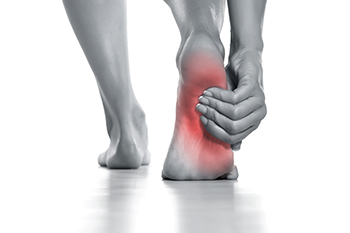
A calcaneal stress fracture is a less common but painful source of heel pain. It often affects people who have recently increased their physical activity, such as starting a new exercise routine or hiking long distances. This type of stress fracture involves microscopic cracks in the heel bone that develop due to repetitive pounding. The pain usually appears gradually, creating a deep, aching sensation, rather than the sharp pain associated with conditions like plantar fasciitis. The pain may worsen with activity, making it difficult to walk without limping. Diagnosing calcaneal stress fractures can be challenging as initial X-rays may not detect the tiny cracks. Advanced imaging, such as MRI scans may be needed. Treatment involves immobilization and restricted weight-bearing for six to eight weeks, often requiring a special boot. If you have heel pain that may have resulted from a stress fracture, it is suggested that you schedule an appointment with a podiatrist.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Daniel Bell, DPM from Florida. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our office located in Pembroke Pines and Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step taken. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Those who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person's bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
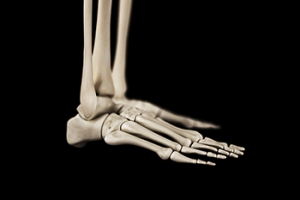
Structure and Function of the Human Foot
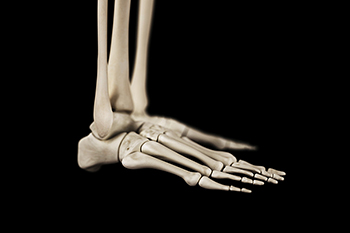
Foot bone anatomy is essential for understanding how the foot supports movement and balance. The foot is divided into three main sections, which are the hindfoot, midfoot, and forefoot. The hindfoot consists of the talus and calcaneus, or heel bone, which play a critical role in weight bearing and shock absorption during walking and running. The midfoot comprises five tarsal bones that provide flexibility and stability, allowing for efficient movement. The forefoot includes the metatarsals and phalanges, which are vital for balance and propulsion. Together, these sections work in harmony to absorb impact, support the body, and facilitate walking, running, and jumping. A strong understanding of foot bone anatomy helps in identifying potential issues and developing effective treatment strategies for foot-related problems. If you have developed a foot condition, it is suggested that you consult a podiatrist who can treat various foot problems.
If you have any concerns about your feet, contact Daniel Bell, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Biomechanics in Podiatry
Podiatric biomechanics is a particular sector of specialty podiatry with licensed practitioners who are trained to diagnose and treat conditions affecting the foot, ankle and lower leg. Biomechanics deals with the forces that act against the body, causing an interference with the biological structures. It focuses on the movement of the ankle, the foot and the forces that interact with them.
A History of Biomechanics
- Biomechanics dates back to the BC era in Egypt where evidence of professional foot care has been recorded.
- In 1974, biomechanics gained a higher profile from the studies of Merton Root, who claimed that by changing or controlling the forces between the ankle and the foot, corrections or conditions could be implemented to gain strength and coordination in the area.
Modern technological improvements are based on past theories and therapeutic processes that provide a better understanding of podiatric concepts for biomechanics. Computers can provide accurate information about the forces and patterns of the feet and lower legs.
Understanding biomechanics of the feet can help improve and eliminate pain, stopping further stress to the foot.
If you have any questions please feel free to contact our office located in Pembroke Pines and Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Biomechanics in Podiatry
Podiatry is a branch of medicine that deals with the study, diagnosis, and treatment of foot and ankle conditions. There are various subdivisions in podiatry; biomechanics is one of them. Biomechanics is the way in which the bones, muscles, and joints of the feet and lower limb interact with each other.
Our feet play crucial roles in the way we move, and it is rare to have feet that are completely symmetrical. Common biomechanical issues include high or low arches or uneven leg heights. Excessive pronation often leads to fallen arches, or flat feet, and is a common cause of running injuries. People whose feet are over-pronated tend to have flexible and unstable feet. Pain is usually experienced during walking and running.
At times, people may be able to adapt to these abnormalities without any difficulties, but in other cases, these issues can cause a great deal of pain. This pain occurs because the joints, muscles, ligaments, and tendons are put under an excess amount of stress during movement. Common symptoms of biomechanical problems stemming from the feet include hip pain, knee pain, leg cramps, ankle pain, lower back pain, weak ankles, tripping, heel pain, Achilles pain, and shin splints.
Many biomechanical issues can be treated with orthotics. Orthotics are shoe insoles that are used to help control the way the foot operates. They can provide relief from foot pain, heel pain, and knee pain. Depending on your specific case, you may need to purchase over-the-counter orthotics or custom orthotics to fit your feet. Your podiatrist will be able to prescribe the perfect orthotic for your feet to help you walk around with ease.
Gait is defined as the way we move our bodies from one point to another. This is usually done by either walking or running. Gait analysis is a method used to assess the way we walk or run to highlight biomechanical abnormalities. Gait analyses are a great way to take a detailed look at how you walk and how your foot moves while you walk. An examination of the feet will help your podiatrist understand why you are suffering pain in other parts of your body.
Benefits of Using Walking Sticks

Walking sticks can be an excellent tool for enhancing stability. They can reduce the risk of falls, particularly for people who have balance problems or for those who walk on uneven surfaces. The additional points of contact with the ground provided by walking sticks can help distribute body weight. This reduces strain on the feet and alleviates pressure that might otherwise lead to pain or even injury. Walking sticks also promote better posture, which reduces foot fatigue during prolonged walks or hikes. When used correctly, walking sticks can assist in maintaining balance and controlling foot movements, which helps minimize slips and trips. It is important to adjust the walking sticks to your height to ensure they provide adequate support for your walking style. A podiatrist can evaluate your specific needs and guide you on whether walking sticks are appropriate for your foot health. If you need an assistive device for walking, it is suggested that you schedule an appointment with a podiatrist who can determine if walking sticks are right for you.
Exercising your feet regularly with the proper foot wear is a great way to prevent injuries and build strength. If you have any concerns about your feet, contact Daniel Bell, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Exercise for Your Feet
Exercise for your feet can help you gain strength, mobility and flexibility in your feet. They say that strengthening your feet can be just as rewarding as strengthening another part of the body. Your feet are very important, and we often forget about them in our daily tasks. But it is because of our feet that are we able to get going and do what we need to. For those of us fortunate enough to not have any foot problems, it is an important gesture to take care of them to ensure good health in the long run.
Some foot health exercises can include ankle pumps, tip-toeing, toe rises, lifting off the floor doing reps and sets, and flexing the toes. It is best to speak with Our doctor to determine an appropriate regimen for your needs. Everyone’s needs and bodies are different, and the activities required to maintain strength in the feet vary from individual to individual.
Once you get into a routine of doing regular exercise, you may notice a difference in your feet and how strong they may become.
If you have any questions please feel free to contact our office located in Pembroke Pines and Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Exercise for Your Feet
Whether your feet are over-worked or under-worked, chances are they could benefit from some special attention. Even those who exercise regularly probably do not spend any time strengthening their feet. This can be just as rewarding as strengthening the rest of the body, since the health of your feet affects the health of the rest of the body as well, especially the ankles, legs, and spine.
For those who might not have any idea on how a foot-specific exercise might be conducted, there are several workouts that are fairly easy to perform in the comfort of ones’ home. One of the easiest is the toe rise, also known as the tip-toe. This exercise involves standing on the tip-toes for a count of 15 then resting the feet on the ground. This process should be repeated a minimum of three times a day in order to strengthen the feet.
Toe pick-ups strengthen the feet by working them in a very different way. In this exercise, small items are picked up using the toes in order to strengthen the muscles on the upper part of the feet. Once again three sets should be performed, with the item in question being held for 15 seconds then dropped. Items that may be picked up using the feet include marbles and even stationery, which works wonders for the toes and the surrounding muscles.
Yet another simple workout is the ankle pump. This can be done either upwards or downwards, but for the workout to be most effective both can be incorporated into the routine. As the term suggests, this involves lifting the foot off the floor and flexing the toes either towards the shin or towards the ground. This movement puts the feet and ankles through a large range of motion which works the muscles.
Last but not least, feet should be stretched so that the muscles can relax and recuperate. This can be done by placing both feet off of the floor and bracing oneself against the wall at a 45 degree angle. This ensures that the feet and ankles are adequately stretched once the workout is complete.
In short, giving the feet a good workout every now and then is important in order to avoid problems such as plantar fasciitis. It’s also important to warm-up or cool-down after running or vigorous walking. Foot exercises may be followed by a good foot massage. This encourages circulation in the feet as well as muscle relaxation.
The Sources of Plantar Fascia Strain
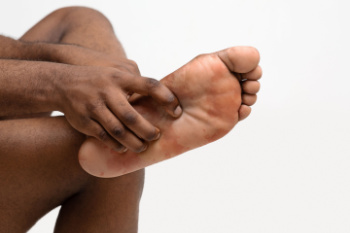
Plantar fasciitis is a common foot condition characterized by inflammation of the plantar fascia, a band of tissue that extends from the heel bone to the toes. This injury often results from repetitive strain, such as from running or sudden increases in physical activity. Prolonged standing, exercising on hard surfaces, and wearing poorly fitting or unsupportive shoes can also contribute to damage. Individuals with flat feet, high arches, are overweight, or are over the age of 40, as well as those with previous foot or ankle injuries, are at higher risk for developing plantar fasciitis. Symptoms typically include heel pain, especially with the first steps in the morning or after periods of rest. Effective management and treatment are key to alleviate pain and prevent further issues. If you are experiencing foot pain or suspect plantar fasciitis, it is suggested you schedule an appointment with a podiatrist.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Daniel Bell, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our office located in Pembroke Pines and Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
Blog Archives
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021